Victoria's testing regime let the virus get away. Here's how to fix it
AdvertisementFor our free coronavirus pandemic coverage, learn more here.
Our brains are hard-wired to look for easy fixes. We buy vitamin pills rather than eating healthily. We expect a vaccine, or the latest wonder drug, to end the pandemic.
LoadingReplay
Replay videoBut even should a vaccine come, there is a realistic chance it won’t stop the virus circulating.
So instead of focusing simply on a cure, we should be imagining how to live in a world where the virus is with us for the long term and focusing on something difficult, unsexy, but utterly crucial to that reality. Something that let us down horribly in Victoria’s second wave: Testing.
Every single other thing you want to do – trace clusters, isolate the infectious, prevent the spread of the virus into nursing homes – is built on testing.
AdvertisementGet it right, and other parts of the pandemic response fall into place.
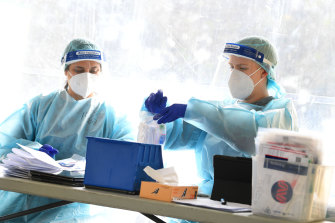
Healthcare workers at a testing facility in Clyde, Melbourne, on September 18.Credit:AAP
Victoria did not get it right. Most of the focus has been on hotel quarantine's failings but authorities knew the virus had breached quarantine and yet they still could not marshall a testing strategy to stop its runaway growth.
Even on Wednesday, people were being turned away from testing queues in Shepparton, suggesting we have not learnt our lesson.
Here's how we can fix it.
Testing times
In May, in those few weeks when it seemed possible that Victoria had the pandemic under control, Shannon Ross’ wife woke up with a sore throat. She went to the local hospital for a test and then bunkered down at home to wait for the results.
Victoria’s testing system should not have been under any strain at all. But it still took eight days for her results to come back. “If something pops up here, we might not know about it until mid-June,” Ross told The Age at the time.
In May, Victoria tested 10,736 people a day. Yet to do that, people had to queue at testing centres for up to three hours.
In June, drive-through sites were overwhelmed, with cars being turned away before centres even opened, the Chief Health Officer urging people to “shop around” for a test site, and overwhelmed diagnostic labs having to ship samples interstate.
Health authorities realised the virus had likely escaped hotel quarantine on May 26. Yet over the next week, the state's 7-day rolling average of tests dropped from 8047 to 6295.
We simply were not testing enough, admits Victoria’s testing commander Jeroen Weimar in an exclusive interview with The Age.
“Our level of testing at the time of seeding was far, far lower. That’s one of the lessons we have had to learn,” he says.
Part of the problem is resourcing. We need to do more tests more often (Weimar hopes to get our testing levels up to 20,000 a day). We did not have enough trained lab techs to do the testing.
"We didn’t have a staff that could perform all these tests without a superhuman undertaking. Exhaustion ensued," says Associate Professor Ian Mackay, a University of Queensland-based testing expert.
But another part of the problem is that our testing regime is not built for a pandemic.
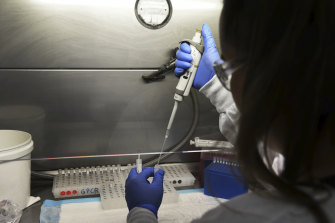
A technical officer at SydPath sets up a coronavirus test.Credit:Kate Geraghty
“Throughput has been something we have seen labs around the world really struggle with. Pandemic plans have not included a PCR-pandemic component,” says Mackay.
What he means is this: the polymerase chain reaction tests which we use are amazing scientific tools but are not built for a pandemic. PCR is extraordinarily accurate, but the version we use takes time, is expensive, and you need to run the test at specialised laboratories.
If you’re trying to stop a quickly spreading virus, speed is vital.
Shannon Ross’ wife did the right thing and stayed home until her results came back. But how many people would wait eight days for a test result? Some of them would go out. Worse, if the result came back positive, contact tracers would be more than a week behind trying to trace any spread.
Victoria currently turns around tests within 48 hours. We could do much better.
Remarkably, a solution already exists: 15-minute GeneXpert PCR test machines are sitting in labs around the country, barely being used.
The machines use small chemical cartridges to rapidly test samples. But with the whole world clamouring for rapid access, Australia doesn’t have enough cartridges.
We have the machines for 15-minute testing, but we don’t have enough ingredients.
“We have really suffered, more than most countries, on a lack of reagents – the things that labs run on,” says Mackay.
That is the sort of problem that can be solved if a government is willing to spend enough. We could outbid other countries or build our own manufacturing capacity.
“It would make a huge difference to the general public,” says Jenny Sikorski, CEO of Public Pathology Australia.
If we are in for the long haul with this virus, we need to think even bigger. What would a gold-standard testing strategy look like?
A layered approach
Victoria’s second wave was triggered by just three security guards from hotel quarantine, each of whom seeded cases into the community before being detected.
Three needles in a 6.65 million-person haystack. To catch that, a single strategy won’t work.
“The most important thing is you have to have multiple strategies,” says Associate Professor Hassan Vally, an epidemiologist at La Trobe University.
Each of those strategies needs to stack on top of the next. The top layer covers a large area at low precision, while the bottom layer should be able to pick out individual cases in a suburb or even a street.
Think of the way a water filter works, with multiple layers of sand, gravel and carbon, each finer than the next. As the wastewater flows through, smaller and smaller pieces of dirt are filtered out.
And wastewater is exactly where Australia’s testing strategy needs to start.

Wastewater testing has emerged as a key early-warning system for COVID-19 outbreaks.Credit:University of Queensland
“We have to have a sewage testing regime,” says Dr Stephen Duckett, director of the health program at the Grattan Institute. “It is cheap and can be done at scale.”
Sick people shed copious amounts of SARS-CoV-2, the virus that causes COVID-19, in droplets washed from their hands, in used tissues flushed down the toilet, even in faeces. This happens before people even know they are sick. And it all ends up in the city’s wastewater. Test the wastewater and you can essentially test the entire city.
At dozens of sites across Australia, scientists have started drawing samples and testing them for SARS-CoV-2’s genetic material.
Early in September, a sample showed up in Apollo Bay’s wastewater, where nobody thought the virus was circling. Testers soon descended en masse. In New Haven, Connecticut, scientists discovered wastewater testing accurately predicted cases and hospital admissions by as much as a week.

A sample showed up in Apollo Bay’s wastewater, where nobody thought the virus was circling.
“I think it’s an extremely effective method. But it only works if there is nearly no virus,” says Associate Professor David Anderson, deputy director of Melbourne’s Burnet Institute.
If the virus is circulating widely, it will also show up across the city’s sewage outflows. But get the virus down to near-elimination, and sewage testing becomes enormously powerful because it can pick out a viral re-emergence before people even know they are sick.
The next testing option is sentinel surveillance. The government could enlist several hundred GP practices across the country in a program of testing every single patient who comes in. It’s a cost-effective way of testing a fairly random sample of Australians.
You could even cluster sentinel sites in known high-risk locations. We already know COVID-19 spreads quickly in more disadvantaged areas, where people live in smaller houses or apartment towers, where work is more likely to be face-to-face, where access to healthcare is lower.
Victoria’s testing strategy involves something similar: we’re going to roll out sentinel testing to high-risk workplaces such as meatworks and aged care facilities. “Those are going to be our bridgeheads,” says Weimar.
But we could go further. We could enlist every GP clinic in disadvantaged areas to become a sentinel testing site.
“You just test routinely, you build it into your existing systems,” says Professor Catherine Bennett, chair of epidemiology at Deakin University.
Since 1994, Australia has operated a sentinel surveillance network for flu. Some 260 GP clinics are part of the network. This could become a permanent COVID-19 detection network. You can even use much the same technology, testing for flu and COVID-19 with a single swab.

“You just test routinely, you build it into your existing systems,” says Professor Catherine Bennett, chair of epidemiology at Deakin University.Credit:Jason South
The spit solution
Of course, sewage testing cannot actually tell you which person in your 100,000-household district is sick. And sentinel surveillance is good for spotting unknown outbreaks, but will miss the vast majority of sick people.
Let’s say you’ve spotted a potential outbreak in a suburb. What then? Testing every single person would take weeks and throw up as many false positives as real results. You’d have no way of knowing if you’d covered 100 per cent of the suburb.
Victoria’s current outbreak strategy is to “flood the place”, in Weimar's words. Hit a hotspot with an overwhelming level of testing. He points to the strategy’s success in containing a rapidly-growing outbreak in the City of Casey in September.
We could go further. Rather than test individuals, you test a suburb street by street. Testers could door-knock every house in a hotspot and ask for a sample of spit.
That spit could be combined into large batches, one per street. Each batch could be quickly tested. Spit tests are less accurate than standard PCR tests but here you’re not trying to find sick people, just zero in on where they are likely to live. Once you have a hit on a street, you can go back and PCR-test every single resident.
“The idea is the households in one area must do it every week,” says Professor Ben Fahimnia, chair of decision sciences at the University of Sydney. “The advantage is currently we need to test every single person. With this one, we don’t need to test every single person.”
Let’s recap: sewage testing and sentinel surveillance let you test broadly. Batch testing lets you hunt through a large group in a single area for infections.
But with COVID-19, not all infections are the same. SARS-CoV-2 is not influenza. It is largely spread in super-spreading events — and those are what we want to catch.
Being a super-spreader may have something to do with biology. You could shed a lot of the virus or be a really loud talker. But most likely they are a result of being in the wrong place at the wrong time.
Think of a highly infectious person with no obvious symptoms walking into a packed pub, meatworks or aged care home.
You need to test in the places where the risk of a super-spreading event is highest. And that test needs to be super-quick; there is little use knowing a super-spreading event happened two days ago.
That’s why many experts believe the future of testing will be rapid. Imagine you’re a meatworker turning up for your shift. You’re met at the front gate by the facility's nurse, who asks you to spit in a tube and wait in your car.
A few minutes later, he or she comes by and gives you the thumbs-up. You’re good to go.
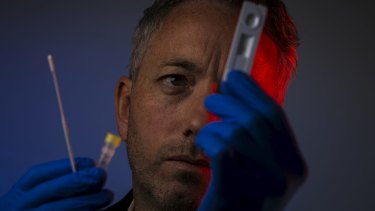
Rapid antigen tests: the future?Credit:Chris Hopkins
These rapid antigen tests, as they are known, are different to normal PCR tests. They cost half as much and don’t need to be sent back to a lab. They look for the presence of viral proteins rather than genetic material. How well they work is not yet clear; the Doherty Institute is testing Australia’s first approved test now, and scientists there caution to be wary of hype.
They are likely to be less accurate than PCR tests. “But in a sense, [PCR tests] are too accurate,” argues economist Professor Richard Holden. “They can pick up incredibly small traces of the virus, including dead virus, so they are not perfectly suited to the question we want to ask which is ‘should a person isolate or not?’."
Because an antigen test picks up virus, not genetic code, Holden says the people it will miss are those who likely only have traces of virus left, meaning they are unlikely to be highly infectious.
Allowing these people to get back to work, rather than quarantine for 14 days, is good for the economy, he adds.
“And you don’t have contact tracers – our scarcest resource at the moment – running around chasing the contacts of someone with dead virus.”
None of these strategies are cheap. But the cost, in some ways, depends on how you think about COVID-19. If it’s a one-off pandemic, it’s expensive. But if you accept the proposition made by scientists who study pandemics that pandemics are only going to get more frequent from here, then developing a world-class testing network looks more like a long-term investment.
“Look at history,” says Weimar. “SARS, MERS, COVID-19. We need to meet the battle we are in, but also the ones further down the road.”
License this articleLiam Mannix
Liam is The Age and Sydney Morning Herald's science reporter
Loading